What Is The Shingles Vaccine
The shingles vaccine can protect you against shingles and postherpetic neuralgia , which is the most common complication of shingles. Shingles is a painful rash caused by the varicella-zoster virus, the same virus that causes chickenpox. The rash usually develops on one side of your body or face. It starts with red bumps and then the bumps turn into fluid-filled blisters.
Who Shouldnt Receive Shringrix
Although vaccines go through rigorous safety testing to ensure they are safe, they arent suitable for everyone. You shouldnt receive Shingrix if you:
- have an active shingles infection
- have a severe illness or a fever of 101.3°F or higher
- have had a severe allergic reaction to Shingrix or any ingredient in the vaccine
- have no immunity to varicella based on a blood test carried out for other reasons
- are pregnant or breastfeeding
If you currently have shingles, another serious illness, or a fever of 101.3°F , wait until these issues have resolved to receive a Shingrix vaccination.
Why Is It Important To Receive A Vaccination Against Shingles
About 33% of adults in the U.S. will develop shingles at some point in their lives. Shingles can cause painful blisters, a rash, chills, and fever, among other symptoms. Many people who have shingles later develop PHN, which can cause long-lasting pain that is difficult to treat.
Getting the Shingrix vaccine can help individuals avoid shingles and PHN and help prevent shingles from spreading to vulnerable people.
Also Check: Is Owens Corning A Good Shingle
Shingrix For Prevention Of Shingles
Shingrix is a vaccine thats used to prevent shingles . Its approved for use in people:
- ages 50 years and older
- ages 18 years and older who have an increased risk of shingles
People with an increased risk of shingles include those with a weakened immune system, such as people with HIV.
Shingrix is not meant for use in preventing chickenpox .
Effectiveness for prevention of shingles
Shingrix has been found to be effective in helping to prevent shingles. For details on how the drug performed in clinical studies, see Shingrixs
state that Shingrix is the preferred vaccine for shingles. They recommend it for:
- all adults ages 50 years and older
- adults ages 18 to 50 years with a weakened immune system
How Safe Is Shingrix
studies showed that Shingrix was safe and effective.
There have been concerns about ingredients, such as thimerosal, that may be added to vaccines. Thimerosal is a kind of preservative that contains mercury. Its added then taken out of some vaccines to keep other germs and bacteria from growing. The concern arose when early research connected thimerosal to autism. This link has since been found to be false. Shingrix doesnt contain thimerosal.
Also Check: Does Priority Health Cover Shingles Vaccine
What Are The Complications Alleged By The Plaintiffs In The Zostavax Lawsuits
Thousands of Zostavax lawsuits have been filed against the drugs manufacturer Merck & Co Inc. Pharmaceuticals since 2016. The plaintiffs in these lawsuits allege that, in addition to the above complications, the administration of Zostavax causes:
- neurological diseases or disorders, like brain inflammation and brain damage,
- spinal cord inflammation ,
- stiffness in the neck and back.3
Encephalitis can be very serious. In extreme cases, it can cause brain damage and death.
Further, treatment of the affliction can be difficult. Patients require extensive care with ongoing monitoring of their heart and respiratory system. Treatment also involves precise management of a persons fluid and electrolyte balances.4
Also Check: Do I Need Prescription For Shingles Vaccine
Assessing Eligibility For Covid
As more people are coming through the doors of vaccine centres, so too are the range of individual circumstances and the queries we are seeing at the Immunisation Advisory Centre to confirm eligibility. The Immunisation Advisory Centre would like to take this opportunity to emphasise that in most cases, the vaccine is safe to deliver. Importantly, vaccination should not be delayed.
It is safe to vaccinate: Pregnant women in any stage of pregnancy People with any medical condition or receiving any type of medical treatment. There are no medical conditions, past or current, or medicines that prevent a person receiving a COVID-19 vaccination. The vaccine is safe for people with compromised immune systems, however they may not have an immune response as strong as a healthy person and it is therefore important for those around them to also have the vaccine. People with history of anaphylaxis as long as it was not caused by the vaccine or something in the vaccine. Vaccinators will discuss this in detail at time of vaccination. People aged 12 years or over for the adult vaccine or 5-11 for the paediatric vaccine. People who are not competent to give consent can be vaccinated if the treatment is seen as in the best interest of the person see guidance set out in the Immunisation Handbook.
For more detailed information please refer to the Immunisation Handbook.
Also Check: Can You Get Shingles If You Have Had The Vaccine
Shingrix And Other Medications
Below are medications that can interact with Shingrix. These are not all the drugs that may interact with Shingrix.
Before taking Shingrix, be sure to tell your doctor and pharmacist about all prescription, over-the-counter, and other drugs you take. Also tell them about any vitamins, herbs, and supplements you use. Sharing this information can help you avoid potential interactions.
If you have questions about drug interactions that may affect you, ask your doctor or pharmacist.
Immunosuppressive drugs such as prednisone
Taking Shingrix with drugs that suppress your immune system can cause problems with the way your body responds to Shingrix. Examples of immunosuppressive medications include:
- corticosteroids, such as:
Here are answers to some frequently asked questions about Shingrix.
Who Should Not Get The Shingles Vaccine
Some people shouldnt get the shingles vaccine. These people include those:
- Who currently have shingles.
- Who have had a severe allergic reaction to the shingles vaccine in the past.
- Who have tested negative for immunity to the varicella-zoster virus, meaning youve never had chickenpox. If youve never had chickenpox, you should get the chickenpox vaccine.
- Who are ill. You should wait until your illness has passed before receiving the shingles vaccine.
- Who are pregnant or breastfeeding.
Read Also: How Do I Catch Shingles
Also Check: How Can I Get Shingles Vaccine Free
Shingles Vaccine: Who Should Get It And When
Shingles is a common viral infection that affects approximately 1 in 3 adults in the United States. It can occur in people of any age who were infected with chickenpox at any time in their life. Usually a childhood disease, chickenpox typically presents with only mild symptoms which may include an itchy, blistering rash, fatigue and fever. Most children recover without incident or complications.
However, once you have had chickenpox, the virus doesnt go away. Instead, it lies dormant within the nervous system without causing any symptoms. If the virus is reactivated, years or decades later, the resulting painful, blistery rash is called shingles.
How Effective Is The Shingles Vaccine In Preventing Shingles
The shingles vaccine can provide strong protection against shingles and postherpetic neuralgia , the most commonly occurring shingles complication.
The shingles vaccine is 97% effective in preventing shingles in people ages 50 to 69 years old. Its 91% effective in people ages 70 years and older.
In addition, the shingles vaccine is 91% effective in preventing PHN in people ages 50 to 69 years old. Its 89% effective in people ages 70 years and older.
Don’t Miss: Does Humana Part D Cover Shingles Vaccine
Pain At Injection Site
Pain at the injection site is a common side effect of many vaccines, including Shingrix. This pain is generally mild but can feel like anything from slight discomfort to deep bruising. In some cases, injection site pain can be severe enough to limit arm movement.
To ease this discomfort, you can apply cold packs to the affected area for 20 minutes at a time.
If these arent effective, over-the-counter pain remedies may help. However, if you have injection site pain that is severe or lasts longer than 2 to 3 days, follow up with your doctor.
Very Common And Common Adverse Events
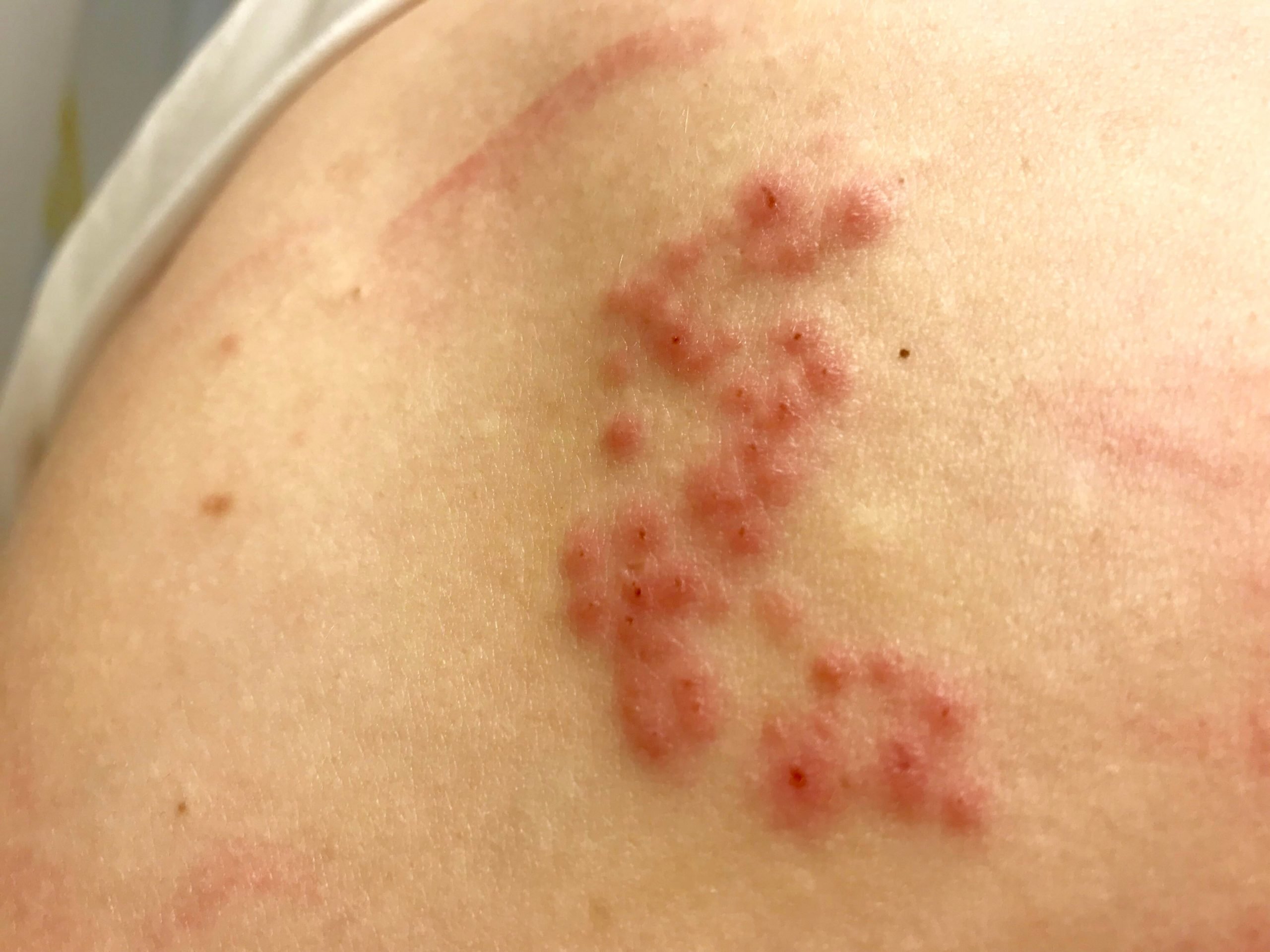
Very common adverse events occur in 10% or more of vaccinees. Common adverse events occur in 1% to less than 10% of vaccinees.
Injection site reactions are very commonly reported for both LZV and RZV. For LZV recipients the frequency is slightly higher in adults aged < 60 years. For all ages, the majority of these events were rated mild or moderate in intensity and lasted less than 2 days.
Due to the adjuvant in RZV, which induces a high cellular immune response and helps address the natural age-related decline in immunity, RZV is more reactogenic than LZV.
Injection site AEs are very commonly reported by recipients of RZV. Approximately 80% report injection-site pain and approximately 30% report redness at the site of injection.
Systemic adverse events, primarily fatigue and myalgia are common in LZV recipients and very common in RZV recipients . For RZV, they include headache .
Local and systemic reactions that were severe enough to interfere with normal activities have been more frequently reported following the receipt of RZV than LZV. However, these reactions have been temporary . Patient education on the short-term reactogenicity of the RZV is recommended prior to vaccine administration to promote adherence to the second dose.
You May Like: What Do You Treat Shingles With
Who Should Get Shingrix
Adults 50 years and older should get two doses of Shingrix, separated by 2 to 6 months. Adults 19 years and older who have or will have weakened immune systems because of disease or therapy should also get two doses of Shingrix. If needed, people with weakened immune systems can get the second dose 1 to 2 months after the first.
You should get Shingrix even if in the past you:
- Received varicella vaccine
There is no maximum age for getting Shingrix.
If you had shingles in the past, Shingrix can help prevent future occurrences of the disease. There is no specific length of time that you need to wait after having shingles before you can receive Shingrix, but generally you should make sure the shingles rash has gone away before getting vaccinated.
Chickenpox and shingles are related because they are caused by the same virus . After a person recovers from chickenpox, the virus stays dormant in the body. It can reactivate years later and cause shingles.
Shingrix is available in doctors offices and pharmacies.
If you have questions about Shingrix, talk with your healthcare provider.
* A shingles vaccine called zoster vaccine live is no longer available for use in the United States, as of November 18, 2020. If you had Zostavax in the past, you should still get Shingrix. Talk to your healthcare provider to determine the best time to get Shingrix.
When Should I Get The Second Dose
The CDC recommends that adults ages 50 and older get a second dose of Shingrix two to six months after their first dose. If youve waited longer than six months since your first dose of Shingrix, its safe to get a second dose right away. Most people dont need to repeat the first dose.
Some immunocompromised adults may need a second dose within one to two months. If you have a disease or are taking medication that affects your immune system, talk to your healthcare provider about the best timeline for your two doses of the shingles vaccine.
Read Also: What Are Shingles On Your Body
Can You Get Shingles After Youve Been Vaccinated
While the shingles vaccine is highly effective, some people can still get shingles. However, people who do get shingles after getting the shingles vaccine usually have milder symptoms and a shorter illness. Youll also be less likely to have complications from shingles, including postherpetic neuralgia.
Also Check: Can You Get The Shingles Vaccine Before Age 50
How Well Does Shingrix Work
Two doses of Shingrix provide strong protection against shingles and postherpetic neuralgia , the most common complication of shingles.
- In adults 50 to 69 years old with healthy immune systems, Shingrix was 97% effective in preventing shingles in adults 70 years and older, Shingrix was 91% effective.
- In adults 50 years and older, Shingrix was 91% effective in preventing PHN in adults 70 years and older, Shingrix was 89% effective.
- In adults with weakened immune systems, Shingrix was between 68% and 91% effective in preventing shingles, depending on their underlying immunocompromising condition.
In people 70 years and older who had healthy immune systems, Shingrix immunity remained high throughout 7 years following vaccination.
Read Also: Should I Get Shingles Vaccine If I Already Had Shingles
Vaccine Safety And Side Effects
Vaccines are very safe, and they can help keep you from getting serious or life-threatening diseases. The most common side effects for all these vaccines are mild and may include pain, swelling, or redness where the vaccine was given.
Before getting any vaccine, talk with a doctor or pharmacist about your health history, including past illnesses and treatments, as well as any allergies. A health care provider can address any concerns you have.
Its a good idea to keep your own vaccination record, listing the types and dates of your shots, along with any side effects or problems.
Who Is At Risk For Shingles Infection
Although it can occur at any age, shingles is more common in older adults and in people with compromised immune systems. In fact, those who are immunocompromised are 1-6 times more prone to infection and have a significantly higher risk of recurrence.
Even people with normal immune systems are at greater risk as they age. Because our immune systems tend to weaken as we get older, by age 50 many people previously infected with chickenpox will have lost the specific immunity they developed after the original infection. When this happens, the virus can wake up and trigger shingles. Some experts believe that chronic stress, some medications and certain health conditions may also trigger the virus to reactivate.
In addition, people who have had COVID-19 are at increased risk. In a recent study, researchers have found that patients over 50 with a history of COVID-19 infection have a 15 percent higher risk of getting shingles, says Dr. Kumar.
Don’t Miss: What Are Some Signs Of Shingles
Shingrix Dosage And Schedule
Shingrix should be administered to immunocompetent adults aged 50 years and older and adults aged 19 years who are or will be immunodeficient or immunosuppressed because of disease or therapy as a two-dose series , 2 to 6 months apart . However, for persons who are or will be immunodeficient or immunosuppressed and who would benefit from completing the series in a shorter period, the second dose can be administered 12 months after the first. See more detailed clinical guidance.
If more than 6 months have elapsed since the first dose of Shingrix, you should administer the second dose as soon as possible. However, you do not need to restart the vaccine series.
If the second dose is given less than 4 weeks after the first dose, the second dose should be considered invalid. A valid second dose should be administered 2 months after the invalid dose .
Live Shingles Vaccine Vs Non
A live vaccine is one that contains a weakened form of a germ. Shingrix is not a live vaccine. Its an inactive vaccine, which is a vaccine thats made from a germ thats been killed.
Because Shingrix is inactive, more people can receive it. This includes people with a weakened immune system .
Zostavax was a shingles vaccine that was live.
People with weakened immune systems are typically advised against receiving live vaccines. This is because on very rare occasions, live vaccines can mutate back to the full-strength germ that causes a disease. If this happens, people with weakened immune systems would have a much higher risk for developing the disease that the vaccine is meant to prevent.
Also Check: Can The Shingles Shot Give You Shingles
No Cure But Strong Prevention
If you get shingles, theres pretty much just two words for it. It sucks. While certain antivirals can help shorten the duration of the virus and may help lessen the pain, theres not much you can do once you have it beyond waiting it out.
There is, however, a lot you can do to ensure you never get it in the first place. The Shingrix vaccinethe second drug to be developed to fight shingles and currently the only one offered in the U.S.has more than a 90% effectiveness rate, says Joshua Zeichner, M.D., an associate professor of dermatology and director of cosmetic and clinical research in dermatology at Mount Sinai Hospital in New York City. That means nine out of 10 people who get the shot will never get shingles, and those who do develop shingles may find the severity of the virus is much less. The vaccine is easy and relatively painless, as far as shots go. The most common side effect from the shingles vaccine is an injection-site reaction, which is redness and swelling in the area that the shot was given, says Dr. Zeichner. Some people may develop general aches, fevers, or chills, but for most patients it does not interfere with daily activities.
The vaccine is just a few years old at this point, so researchers are still exploring how long it protects you from shingles. Unlike the flu vaccine that is recommended as an annual shot, the shingles vaccine is believed to work for up to four years.
Uncommon Rare And Very Rare Adverse Events
Uncommon adverse events occur in 0.1% to less than 1% of vaccinees. Rare and very rare adverse events occur, respectively, in 0.01% to less than 0.1% and less than 0.01% of vaccinees.
Both HZ vaccines are safe with serious adverse events reported very rarely in immunocompetent individuals.
Recurrence or exacerbation of herpes zoster ophthalmicus following LZV vaccination has been reported very rarely, involving several cases world-wide following LZV immunization. Following a causality assessment of seven cases of HZO which were temporally associated with the administration of LZV, NACI concluded that there was insufficient evidence to recommend for or against the administration of LZV in individuals with a history of HZO. More evidence is required for further assessment of risk related to HZO recurrence in LZV recipients. At this time, there is insufficient evidence to assess the risk related to HZO recurrence following RZV recipients.
See Contraindications and Precautions if considering vaccinating a person with previous HZO.
For more information, refer to Adverse Events Following Immunization in Part 2 and the product monograph in Health Canada’s Drug Product Database.
Recommended Reading: How Long Between Shingles Vaccine Doses