How Is Shingles Diagnosed
Most of the time, a healthcare professional can diagnose shingles by performing a physical exam, including an examination of the eyes to see if theyve been affected.
Shingles may be harder to diagnose if the rash is spread out over a large portion of the body or has an unusual appearance. If thats the case, the healthcare professional can take skin samples from a lesion and send them to a lab for cultures or microscopic analysis.
So What Does This Tell Us
In the past, we might have reasonably presumed that a person presenting with a serious, HIV-related illness was simply infected years ago and was only just now becoming symptomatic.
We now understand that, in some patients, serious disease can accompany even the earliest stages of infection.
Even more surprisingly, we now know that these conditions tend to occur in patients with healthier immune systems. According to the research, individuals with a stronger immune response were more likely to experience a severe acute episode than someone with a moderately suppressed system.
While the mechanisms for these disorders are not entirely clear, we do know that certain factors can increase their likelihood, including an extremely high viral load in early infection and the type of virus the person is infected with .
We are also gaining greater insight into the rate and extent of HIV infiltration in the gut and brain, and the factors that might predispose a person to serious gastrointestinal and central nervous system infections.
The research strongly supports HIV testing of all Americans ages 15 to 65 as part of a routine doctor’s visit. No longer can we presume a person to be at low risk simply because they are not presenting with classical signs of infection.
HIV Doctor Discussion Guide
Hiv And Herpes Zoster
HIV indicator conditions are conditions or symptoms that occur more often in people with an underlying HIV infection than in people without an HIV infection. Herpes zoster is one of the HIV indicator conditions. If you have or have had Herpes zoster and have not been tested for HIV, it is advisable to ask your doctor or general practitioner for an HIV test. Find it difficult to ask for an HIV test? You may download a call card that will help you formulate your question.
Recommended Reading: What Does Shingles Look Like On Your Chest
Immune Reconstitution Inflammatory Syndrome
At times, shingles flares up after people with HIV start treatment. This is due to a mechanism called immune reconstitution inflammatory syndrome, or IRIS. IRIS is a state of a hyperinflammatory response, a complication as a result of antiretroviral therapy , and usually happens within the first six months of treatment.
If someone develops shingles shortly after beginning treatment for HIV, this may show that the immune system is responding to treatment by targeting specific viruses and bacteria in the body. This is known as immune restoration syndrome. If you suspect shingles after starting ART, talk to your doctor immediately to lower your chances of developing shingles-related complications.
What Are Early Signs Of Shingles
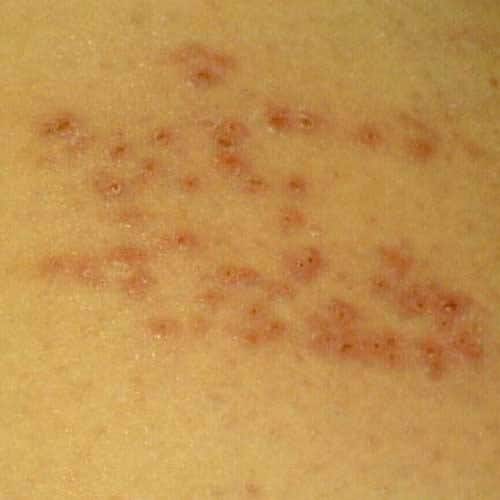
Early signs of shingles produce symptoms similar to a usual viral infection. The distinctive shingles rash may take days to appear despite itching and pain at the site of infection. This can lead to a missed or prolonged diagnosis. However, there are other early signs of shingles to look out for, including:
You May Like: What Does Cvs Charge For Shingles Vaccine
When To Seek Medical Care
Early diagnosis is key. If you think youve been exposed to HIV or have an encounter that put you at risk for HIV, you should seek medical care right away with a primary care doctor, urgent or walk-in clinic, or, if those are not available to you, a local emergency room.
Doctors can give you a medication called post-exposure prophylaxis after exposure to reduce your chances of developing HIV. But this medication needs to be taken within 72 hours of exposure. Ideally, youd start taking it within the first 24 hours.
If you think you were exposed to HIV in the past for example, if a former sexual partner tells you they have HIV its critical to seek medical care as soon as possible. The sooner you find out you have HIV, the sooner you can start treatment.
Why Shingles May Be A First Sign Of Hiv
Research indicates that shingles may actually be an early sign of human immunodeficiency virus . HIV is also associated with a more severe case of shingles, in addition to other complications like long-lasting pain. In this article, we’ll discuss the connection between HIV and shingles.
Chokchai Silarug / Getty Images
Recommended Reading: How Many Shots For Shingles Vaccine
What Are The Symptoms Of Shingles
The most obvious symptom of shingles is a rash that usually winds around one side of the back and chest.
Some people start to feel a tingling sensation or pain several days before the rash appears. It begins with a few red bumps. Over the course of 3 to 5 days, many more bumps form.
The bumps fill with fluid and turn into blisters, or lesions. The rash may sting, burn, or itch. It can become very painful.
After a few days, the blisters begin to dry out and form a crust. These scabs usually start to fall off in about a week. The whole process can take 2 to 4 weeks. After the scabs fall off, subtle color changes may be visible on the skin. Sometimes the blisters leave scars.
Some people experience lingering pain after the rash clears up. This is a condition known as postherpetic neuralgia. It can last several months, though in rare cases the pain remains for years.
Other symptoms include fever, nausea, and diarrhea. Shingles can also occur around the eye, which can be quite painful and may result in eye damage.
For symptoms of shingles, see a healthcare professional right away. Prompt treatment can cut down on the risk of serious complications.
First Stage: Acute Hiv Infection Symptoms
Most people don’t know right away when they’ve been infected with HIV. But they may have symptoms within 2 to 6 weeks after theyâve gotten the virus. This is when your body’s immune system puts up a fight. It’s called acute retroviral syndrome or primary HIV infection.
The symptoms are similar to those of other viral illnesses, and they’re often compared to the flu. They typically last a week or two and then go away. Early signs of HIV include:
- Headache and other neurological symptoms
If you have symptoms like these and might have come into contact with someone with HIV in the past 2 to 6 weeks, go to a doctor and ask that you get an HIV test. If you donât have symptoms but still think you might have come into contact with the virus, get tested.
Early testing is important for two reasons. First, at this stage, levels of HIV in your blood and bodily fluids are very high. This makes it especially contagious. Second, starting treatment as soon as possible might help boost your immune system and ease your symptoms.
A combination of medications can help fight HIV, keep your immune system healthy, and keep you from spreading the virus. If you take these medications and have healthy habits, your HIV infection probably wonât get worse.
Don’t Miss: What Is Shingles And What Causes It
What Are The Health Complications
The most common complication of shingles is postherpetic neuralgia . PHN causes severe pain even after the shingles rash clears.
People aged 60 years and older who dont seek treatment for shingles are more likely to develop PHN.
Shingles can also cause serious sight problems if it infects the structures of the eye.
Other rare complications include:
Hiv Prevalence In Patients With Herpes Zoster
Correspondence Address
| How to cite this article: Kar P K, Ramasastry C V. HIV prevalence in patients with herpes zoster. Indian J Dermatol Venereol Leprol 2003 69:116-119 |
Abstract
Keywords:
Introduction
Herpes zoster, due to reactivation of varicella-zoster virus infection, is associated with depression of immunity. Herpes zoster has been reported in various immunodeficiency states, in lymphoma/leukaemia and other cancers, after organ transplantation, and during chemotherapy., Before the discovery of the human immunodeficiency virus , the development of herpes zoster was noted in homosexual men., Lately, results of sero-epidemiological studies have suggested that herpes zoster is associated with HIV infection.,
The incubation period between HIV infection and the development of herpes zoster is, in most cases, several years,, but due to continuous decline in immunity, herpes zoster may appear shortly after seroconversion., Assuming herpes zoster is a part of the clinical spectrum of HIV infection, we speculated that zoster might be a pointer to declining immunity, although lesser than it would be in full blown acquired immunodeficiency syndrome . To test these hypotheses, we investigated the incidence of HIV seropositivity in men suffering from herpes zoster.
Materials and Methods
Results
In the 11 seropositive patients with herpes zoster the dermatomal areas included trigeminal thoracic, thoracolumbar, and lumbosacral region.
Sexual behaviors
Complication
Discussion
Also Check: How To Stop Shingles Early
Appearance Of The Shingles Rash
The eruptive stage of shingles begins a few days later. This is when a rash appears.
The skin in the area of the prodromal pain caused by shingles will often be sensitive to the touch and reddish in appearance. As these symptoms get worse, it may begin to feel like a sunburn.
Within three to five days of the initial pain, a few tiny pimple-like spots appear and quickly multiply into clusters, forming a rash that feels prickly to the touch.
From there, sometimes within hours, the pimples develop into water-filled blisters, or vesicles, that then consolidate into larger blisters. Often, redness and swelling accompany the rash.
The shingles rash looks very much like the chickenpox rash, with a key difference: Chickenpox blisters are widely scattered over the entire body. With shingles, the rash almost always occupies a finite strip of skin.
Ultimately, the pain of shingles may get so excruciating that simply grazing the skin with clothing can set off what feels like an electric shock.
Symptom : Fatigue And Headache
The inflammatory response generated by your besieged immune system can cause you to feel tired and lethargic. Sometimes it can make you feel winded while walking or generally feel out of breath. Fatigue can be both an early and later symptom of HIV.
There are several things that can cause a person to feel fatigued, so pay attention to your body and your lifestyle to see if you can draw a conclusion. If your fatigue persists, seek advice from your doctor.
Also Check: Topical Treatment For Shingles Pain
Symptom : Swollen Lymph Nodes Achy Muscles And Joint Pain
Lymph nodes are part of your bodys immune system and protect your blood by getting rid of bacteria and viruses. They tend to get inflamed when theres an infection. Many of them are located in your armpit, groin and neck which can result in aches and pains in these areas.
Given these symptoms are common across many viral infections, they alone are not a reliable way to determine if the infection you are experiencing is HIV.
What Is The Treatment For Hiv
Individuals who are HIV positive will likely need to see a specialist. As with many other conditions, early detection offers more options for treatment. Today, there are medical treatments that can slow down the rate at which HIV weakens the immune system. However, there are other treatments that can prevent or cure the conditions associated with HIV. Anti-retroviral drug therapy may be given to a pregnant woman, which has proven to greatly reduce the chance of an infant developing HIV. A cesarean section may be recommended to reduce infant transmission from the birth canal. In the U.S., where other feeding options are available, an infected mother should be discouraged from breastfeeding her infant. Consult your child’s doctor for more information regarding various drug therapies.
Recommended Reading: Does Cvs Do Shingles Shots
Hiv Rashes Caused By Medication
Drugs that treat HIV and related infections can trigger rashes. These often go away several days or weeks after you stop taking the drug. Talk with your doctor before stopping any medication.
If you have a rash along with fever, fatigue, headache, muscle pains, upset stomach, vomiting, and belly pain, you might have a âhypersensitivity reaction,â which can happen with several HIV medications, including:
- Abacavir and medications that have abacavir in them
- Dolutegravir and medications that have dolutegravir in them
What Are The Treatment Options For Shingles
Treatment for shingles is the same regardless of whether a person has HIV. Treatment includes the following:
- getting started on an antiviral medication as quickly as possible to ease symptoms and potentially shorten the duration of the illness
- taking an over-the-counter or prescription pain reliever, depending on how severe the pain is
- using an OTC lotion to relieve itching, being sure to avoid lotions that contain cortisone
- applying a cool compress
Eye drops that contain corticosteroids can treat inflammation in cases of shingles of the eye.
Lesions should be examined by a healthcare professional right away.
Also Check: What Is The Course Of Shingles
Where A Shingles Rash Forms
A shingles rash typically occurs on the face, neck, or chest, on just one side of the body.
The affected area of skin is called a dermatome, a region supplied by the sensory fibers of a specific spinal nerve. Outbreaks can involve two adjacent dermatomes, but rarely two non-adjacent dermatomes.
The exception may be in people whose immune systems are severely comprised, such as those with advanced HIV infection. They’re often at risk of disseminated shingles , shingles of the eyes or internal organs, and a recurrence of shingles within six months.
What Is An Aids
These are conditions which are very rare in people who do not have AIDS . Pneumocystis is an AIDS-defining illness, therefore anyone presenting with pneumocystis pneumonia almost certainly has AIDS. Certain malignancies such as Kaposis sarcoma and non-lymphoid lymphoma are also AIDS-defining illnesses.
Recommended Reading: What To Use For Shingles Itching
Dhhs Guidelines For Antiretroviral Agents
Current Guidelines for the Use of Antiretroviral Agents in HIV-1Infected Adults and Adolescents, published by US Department of Health and Human Services, recommend starting antiretroviral therapy for all individuals when infection is diagnosed, regardless of stage of infection, as long as barriers to therapy do not exist. Considerations are as follows:
-
The goal of treatment should be the suppression of plasma HIV RNA to below detectable levels
-
Testing for plasma HIV RNA levels and CD4 count and toxicity monitoring should be performed
-
If therapy is initiated before drug-resistance test results are available, a ritonavir-boosted protease inhibitorbased regimen should be used, because clinically significant resistance to protease inhibitors is less common than resistance to non-nucleoside reverse transcriptase and integrase inhibitors in antiretroviral therapynaive persons who harbor drug-resistant virus.
Treatment Initiation According To Cd4 Count
In 2008, a subset analysis of the Strategic Management of Antiretroviral Therapy study found that although deferring treatment until the CD4+ T-cell count dropped below 200 cells/µL had been the standard of care, initiation of combined antiretroviral therapy at higher CD4 counts was associated with decreased morbidity and mortality in HIV disease.
Similarly, the National Institutes of Health Comprehensive International Program of Research on AIDS HT 001 clinical study showed that starting antiretroviral therapy at CD4 T-cell counts between 200-350 cells/µL improves survival compared with deferring treatment until the CD4 T-cell count drops below 200 cells/µL, which was the standard of care at the time.
Interim analysis of CIPRA HT 001 showed that of 816 HIV-infected adults with early HIV disease, 6 of those who began antiretroviral therapy within 2 weeks of enrollment died, whereas 23 participants in the standard-of-care group died. Among participants who began the study without tuberculosis infection, 18 individuals in the early treatment group developed tuberculosis, whereas 36 people in the standard-of-care group developed tuberculosis.
These interim results were statistically significant and led to ending the trial early to offer antiretroviral therapy to all participants in the standard-of-care group with a CD4+ T-cell count of less than 350 cells/µL.
Don’t Miss: Rosen Shingle Creek Hotel Orlando Fl
Assessing Immunity To Varicella
Two doses of varicella vaccine are recommended for all children, adolescents, and adults without evidence of immunity to varicella. Those who previously received one dose of varicella vaccine should receive their second dose for best protection against the disease.
Evidence of immunity to varicella includes any of the following:
- Documentation of age-appropriate varicella vaccination
- Preschool-age children : one dose
- School-age children, adolescents, and adults: two doses
*Commercial assays can be used to assess disease-induced immunity, but they lack sensitivity to detect vaccine-induced immunity .
To verify a history of varicella, healthcare providers should inquire about:
- An epidemiologic link to another typical varicella case or to a laboratory confirmed case, or
- Evidence of laboratory confirmation, if testing was performed at the time of acute disease
People who have neither an epidemiologic link nor laboratory confirmation of varicella should not be considered as having a valid history of disease. For these people, a second dose of vaccine is recommended if they previously received only one dose. If a healthcare provider verifies the diagnosis based on the above criteria, then vaccination is not needed.
Treatment Of Acute Hiv Infection
Antiretroviral treatment of chronic HIV infection is well supported and widely recommended. ART for acute HIV infection is controversial. However, treating acute HIV infection has several theoretical advantages, as follows :
-
To relieve symptoms in some symptomatic patients
-
To halt viral evolution at a time of minimal viral diversity, prior to viral adaptations to specific host immune responses
-
To protect developing immune responses from the deleterious effects of sustained HIV viremia
-
To reduce the viral set-point
-
To limit the latent pool of infection
Several studies have shown no benefit for short-term combination antiretroviral therapy during acute infection. However, a 2006 retrospective study found that an initiation of combination therapy within 2 weeks of HIV seroconversion was associated with sustained viral load and CD4 cell count benefits for up to 72 weeks after termination of therapy.
In 2007, another group found that in patients who received 3 months of antiretroviral therapy, the subsequent CD4 cell count decline over 3 years was slower than in patients who did not receive acute therapy. When antiretroviral therapy was started later than 2 weeks after antibody seroconversion, however, patients had a persistent but decreasing CD4 T cell count benefit and a loss of the viral load benefit by week 72 after discontinuation of treatment.
CD4 cell counts appear to deplete very rapidly during acute HIV infection.
Don’t Miss: Can You Get A Mild Case Of Shingles